
The Setting
You’re on a backcountry ski trip with 4 friends, and currently a four-hour ski from the nearest road. The weather over the last 24 hours has been challenging, with unanticipated daily highs of 9°F (-12°C) and nighttime lows of -20°F (-28°C).
When you stopped to camp one of your companions revealed that they may have frostbite on their fingers. As the Wilderness First Responder (WFR) in the group, you asked if you could look at their hands. You were struck by how white they looked, especially the fingers on the right hand.
SOAP Report
Subjective
The patient is a 24-year-old with possible frostbite to their right fingers.
Objective
Patient Exam
The patient’s distal joints of the fingers of their right hand are white, numb and hard. The remainder of the hand is cool, pale and soft. There is no injury to the right thumb, left hand/fingers or to the feet. The patient is not hypothermic.
Vital Signs
|
Time |
4:00pm |
|
Level of Responsiveness (LOR) |
A+O x4 |
|
Heart Rate (HR) |
92, strong, regular |
|
Respiratory Rate (RR) |
16, easy, regular |
|
Skin Color Temperature Moisture (SCTM) |
Mucous membranes are pink, skin is warm, dry (except right hand) |
|
Blood Pressure (BP) |
radial pulses present |
|
Pupils |
PERRL |
|
Temperature (T) |
99°F (37.2°C) oral |
Patient History
|
Symptoms |
Denies. |
|
Allergies |
None. |
|
Medications |
Ibuprofen 400mg three times today for muscle aches. |
|
Pertinent History |
No previous cold injury history, no relevant medical history. |
|
Last in/out |
Patient is well hydrated, has been eating throughout the day, normal urine and bowel function. |
|
Events |
Patient was skiing in cold weather and had trouble keeping their hands warm. |
Stop Reading!
What is your assessment and plan? Take a few minutes to figure out your own assessment and make a plan. Don’t cheat—no reading on without answering this first!

Assessment
-
Possible frostbite to the fingers of the right hand.
Plan
-
Set up camp.
-
Make a decision whether to try to thaw the fingers.
-
Evacuate tomorrow.
Anticipated Problems
If we thaw the fingers we will need to keep them warm and protected from injury during the evacuation. Tomorrow’s temperature prediction is for highs not reaching 0°F (-17°C).
Notes from NOLS on Frostbite:
In an urban setting, frostbite is thawed in the emergency room. In the wilderness a critical decision is whether to thaw in the field. Things to consider in making this decision:
- The ideal treatment for frostbite is rapid thawing by immersion in a warm water bath.
- Tissue damage seems to be related to the length of time the tissue stays frozen. How long tissue can be kept frozen without increasing damage is unknown.
- Refreezing thawed tissue causes significantly worse injury.
- Thawing will be painful.
- The thawed tissue will be unusable and must be protected from injury, as well as kept warm. Thawed toes may make it impossible to walk or ski. Thawed fingers may not be usable to climb or hold a pole.
- Most frostbite will thaw spontaneously, and slowly, especially if the patient is taken to shelter and treated for hypothermia.
The Tale Continues
You explained the situation and the decision-making parameters to the patient and your companions. The patient agreed that their fingers would likely thaw slowly now that they are warm and in shelter. The patient anticipated they could ski to the road tomorrow with one pole and without a pack. They agreed to the warm water bath.
Before immersing their hand in water, you removed a ring from their index finger and a bracelet from their wrist. The patient immersed the fingers of their right hand into the pot of warm water after we tested it and estimated it as warm bath water. The pain was intense. The patient was only able to tolerate the procedure for 15 minutes. Assessment at that point showed the fingers were pink and warm to the end of the digits.
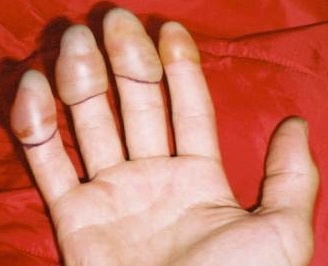
The fingers were kept warm through the night. At dawn the fingertips were pink and painful. Clear fluid blisters had formed overnight on all four fingers extending from the last joint about two-thirds of the way to the fingertip. The patient took 800 mg ibuprofen every four hours through the night. They rated the pain at 7 on a 1-10 scale.
Before skiing out, you dressed the fingers lightly with gauze and protected them from the cold with two spare socks and one large expedition over-mitten. You began to ski with the hand in a sling and swathe, but this made the patient unbalanced. You completed the ski without the patient falling by allowing their arm hang free to move, but not using a ski pole. The fingers remained warm throughout. The blisters did not grow larger or rupture.
End of the Tale
The patient healed well. They eventually lost their fingernails, but no other tissue. They returned to winter camping with a heightened resolve not to tolerate cold fingers or toes.
Stay ready to respond: recertify your WFA, WFR, or WEMT with NOLS.
Written By
Tod Schimelpfenig
As a NOLS Instructor since 1973 and a WEMT, volunteer EMT on ambulance and search and rescue squads since the 70s, Tod Schimelpfenig has extensive experience with wilderness risk management. He has used this valuable experience to conduct safety reviews as well as serve as the NOLS Risk Management Director for eight years, the NOLS Rocky Mountain Director for six years, and three years on the board of directors of the Wilderness Medical Society, where he received the WMS Warren Bowman Award for lifetime contribution to the field of wilderness medicine. Tod is the founder of the Wilderness Risk Manager’s Committee, has spoken at numerous conferences on pre-hospital and wilderness medicine, including the Australian National Conference on Risk Management in Outdoor Recreation, and has taught wilderness medicine around the world. He has written numerous articles on educational program, risk management and wilderness medicine topics, and currently reviews articles for the Journal of Wilderness and Environmental Medicine. Additionally, he is the author of NOLS Wilderness Medicine and co-author of Risk Management for Outdoor Leaders, as well as multiple articles regarding wilderness medicine. Tod is the retired curriculum director for NOLS Wilderness Medicine and is an active wilderness medicine instructor




