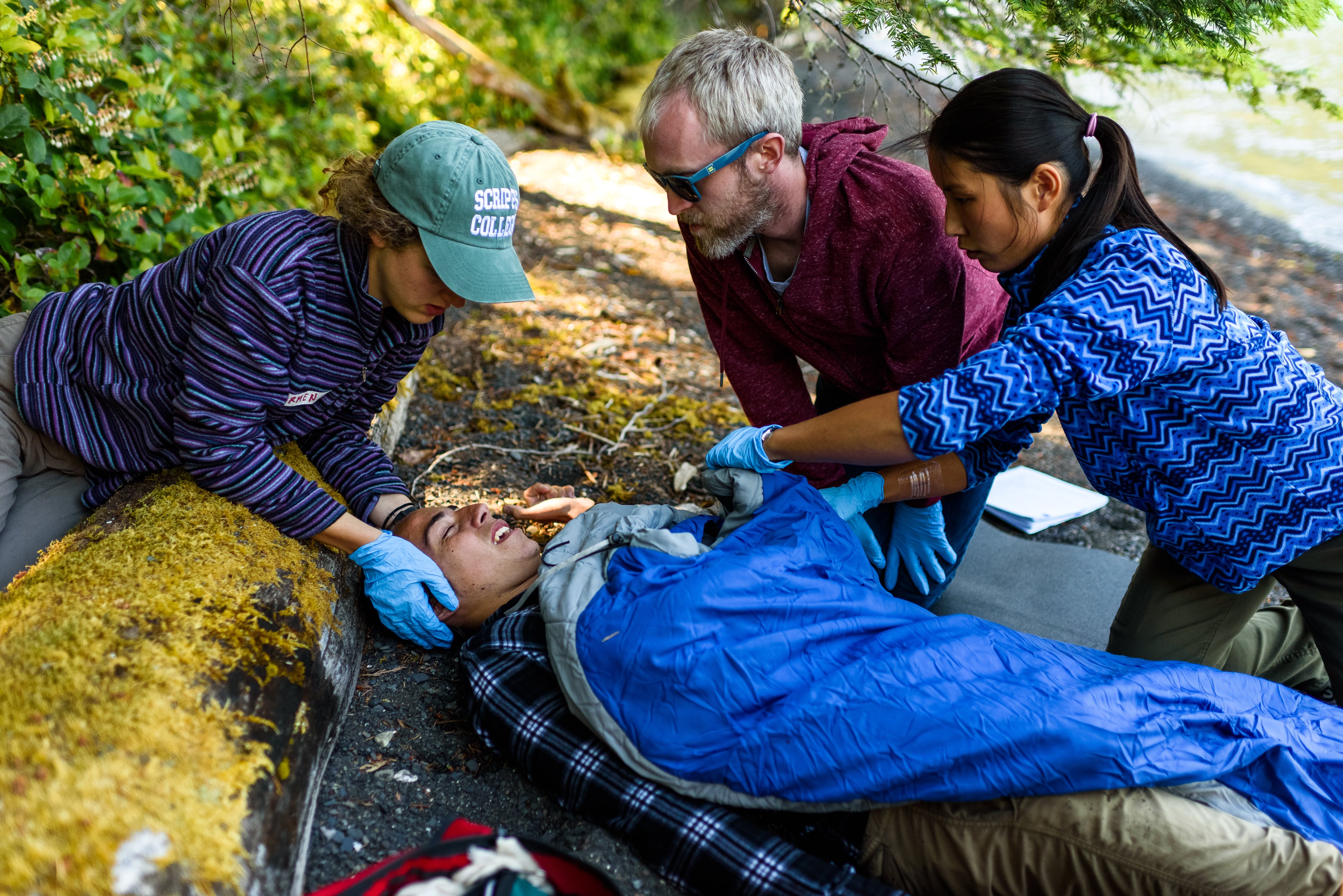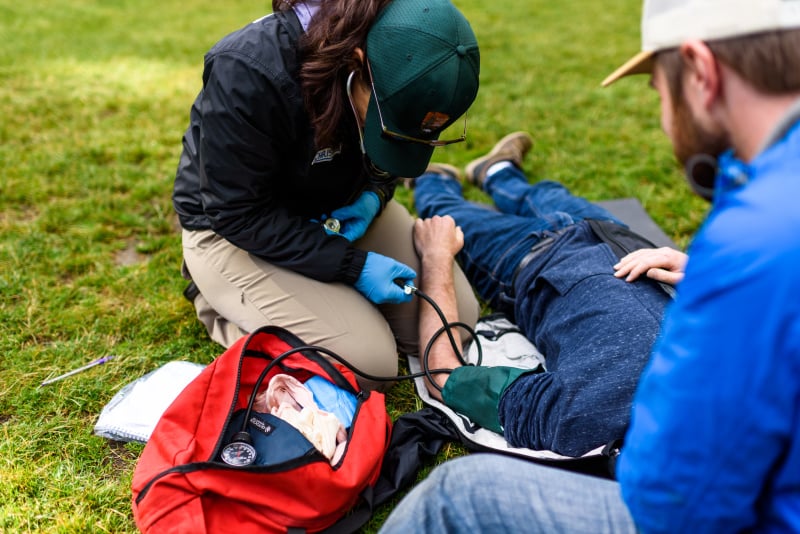
You’ve taken your WFA, WFR, or WEMT and learned about PAS, ABCDE, and MOI. So many abbreviations, so little time!
Whether you’re filling out a SOAP note for a real-life patient or reviewing your skills with a NOLS case study, wilderness medicine’s plethora of abbreviations and acronyms can be a lot to remember.
To help you better understand the world of wilderness medicine (or review for your next recertification), here are the top 9 need-to-know abbreviations.
PAS: Patient Assessment System

What is it?
A systematic approach to collecting information about a patient's complaints or concerns.
This is a tool, sometimes displayed as a pyramid, used for checking for life-threatening problems, surveying the patient for injury and illness, and gathering the information needed to prioritize treatment and evacuation decisions.
Key elements of the PAS include: scene size-up, initial assessment, secondary assessment (patient exam, patient history, vital signs), and using these assessments to make a plan.
ABCDE: Airway, Breathing, Circulation, Disability, Environment/Expose

What is it?
A memory aid for identifying and fixing immediate threats to life, which is part of your initial assessment of a patient.
- Airway: Make sure the mouth, nose, throat, and upper airway are clear of obstructions so the patient can breathe.
- Breathing: Look, listen, and feel for breathing. Are they breathing? Is the breathing labored, easy, deep, shallow, etc.?
- Circulation: Check for a pulse and look for signs of severe bleeding.
- Disability: Making a decision if spine protection is needed (if you didn’t observe the incident, assume disability).
- Expose: Examine your patient for obvious, major injuries, and if needed control bleeding.
MOI: Mechanism of Injury
What is it?
The method by which the patient's injury occurred.
What happened? Was the patient wearing a helmet or other protective equipment? If they fell, how far? Did they land on soft ground, snow, or rocks? Did they free fall or tumble?
Asking questions like these about the MOI can give you critical information about the location and severity of injuries.
CSM: Circulation, Sensation, Motion

What is it?
Three extremity assessments that must be completed to assess for good sensory, neurological, and motor function.
- Circulation: Check the radial pulse in each hand and pedal pulse on each ankle—they should be equal on both sides. Another option is to check to see if their hands and feet are warm.
- Sensation: Gently squeeze one of the patient’s fingers and toes toward the outside of each foot or hand and one toward the inside of each foot or hand, and ask them to identify each digit in question.
- Motion: Ask your patient to move their fingers or toes, and test grip strength by having the patient squeeze your hands.
SAMPLE: Symptoms, Allergies, Medications, Pertinent History, Last Intake/Output, Events
What is it?
A memory aid to guide questions while taking a patient's medical history.
- Symptoms: What symptoms is the patient showing?
- Allergies: To things like environmental factors, insects, medications, or food.
- Medications: Ask about any medications, including prescription and over the counter medicines.
- Previous/Pertinent: Ask about their medical history to discover any pertinent, prior events related to the current injury or illness.
- Last intake/output: When was the last time the patient ate, drank, urinated, and defecated?
- Events: What has led up to the incident in the last few days? Gathering this information is crucial to your assessment and plan for handling the situation.
SCTM: Skin Color, Temperature, Moisture
What is it?
The three elements to assess while taking the skin vital sign. Skin signs indicate the condition of the respiratory and cardiovascular systems.
- Skin Color: For lighter-skinned people, pinkness is normal. In darker-skinned people, skin color can be assessed at the nail beds, inside the mouth, palms, soles of feet, or lips.
- Temperature: Can be assessed at the forehead, hands, and trunk. In a healthy person, skin is warm and relatively dry.
- Moisture: Combined with temperature, like cool, clammy skin or hot, dry skin, the level of moisture can indicate various stressors on the body.
BSI: Body Substance Isolation
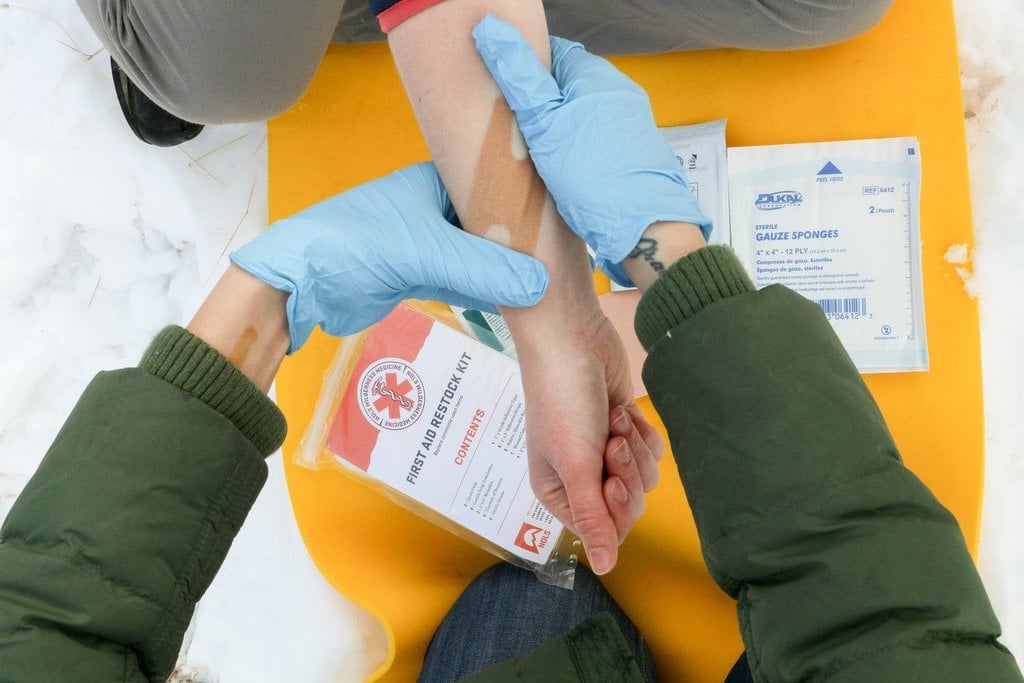
What is it?
Taking appropriate steps to protect yourself from infectious disease transferred from a patient’s body fluids and tissues.
Protect yourself by washing your hands, using gloves, eyewear, and face masks, and properly disposing of soiled bandages, dressings, and clothing.
Disposable gloves are a crucial part of BSI that should be in your first aid kit. Wear them when there is a chance you may contact a patient’s blood, other bodily fluids, mucous membranes, or broken skin.
LOR: Level of Responsiveness

What is it?
A way to assess, brain function, or mental status, based on how responsive a patient is to their environment.
LOR can be affected by toxic chemicals, drugs or alcohol, low blood sugar, abnormally high or low temperature, shock, and more.
Assessing your patient’s LOR means checking to see if they are awake and oriented to who they are, where they are, what date or time it is and recent events. It can also mean checking if the patient is responsive to verbal stimuli, responsive to pain, or totally unresponsive.
SOAP Note: Subjective, Objective, Assessment, Plan
What is it?
A SOAP note is a widely used method of documentation for healthcare providers.
Writing down the results of your assessment in the organized format of a SOAP note can help develop your treatment and transport plan, communicate with evacuation or rescue parties, and pass on information to healthcare professionals when you transfer a patient.
- Subjective: This information is told to you by patients or bystanders, such as the order of events
- Objective: This information is measurable and observable, like vital signs.
- Assessment: categorizes the patient’s medical concerns as a problem list.
- Plan: Will note treatments for each problem and additional action steps.
Keep your skills fresh: Recertify with NOLS
Editor’s Note: When communicating, especially in an emergency, it’s best to use plain language and not assume these acronyms and memory aids are universal.
Written By
Ben Lerman
Ben is the former NOLS Wilderness Medicine Marketing Coordinator and a Wilderness First Responder graduate. He enjoys rock climbing, backpacking, kayaking, and hopes to someday adventure in the mountains on each of the 7 continents.