
What is shock? It’s a term that gets used frequently in casual conversation to describe emotional reactions. It’s also a serious medical condition that can be difficult to recognize, and even harder to treat, in the wilderness context.
Myth Busting
Myth: People can go into shock from witnessing a traumatic event, like seeing lots of blood at an accident scene.
The reality? “Although a highly stressful event may indeed be shocking, it does not cause medical shock. Medical shock results from a problem with the circulatory system. Specifically, it is the inadequate perfusion of tissues with oxygenated blood. In other words, when there is a problem with the heart, the blood vessels, and/or the blood, the body can go into shock.” —Ben Tettlebaum, NOLS Wilderness Medicine Instructor
Cardiologist Dr. Bruce Paton uses the following analogy for shock in NOLS Wilderness Medicine:
“Imagine the body as a healthy wetland with a river running through lush vegetation. The vegetation depends on the river’s flow of pure, unpolluted water and the nutrients it carries. If the river dries up or the water becomes poisoned, the plants shrivel and die.”
In the same way, the body depends on healthy, well-oxygenated blood flowing through the tissues. If the circulatory system fails, causing life-threatening cardiovascular shock, bodily processes slow and tissue begins to die. Shock is often the lethal component that accompanies extensive burns, injuries to the chest and abdomen, severe bleeding, and other serious illnesses and injuries that disrupt the circulatory system.
Early Signs and Symptoms
- Rapid and/or weak pulse
- Rapid and/or shallow breathing
- Pale, cool, clammy skin
- Anxiety or restlessness
- Nausea, thirst
These early changes related to shock are similar to the body’s “fight or flight” response to danger or stress. If your patient is not seriously ill or injured and their circulatory system is healthy, this stress reaction should abate in a short time (review the components of psychological first aidfor appropriate responses to stress reactions).
If the circulatory system is unable to adjust due to shock, a downward spiral of deterioration may begin, resulting from a lack of oxygen getting to important bodily systems.
Treating Shock
You must anticipate, recognize, and treat every patient for shock until it can be ruled out. This is especially necessary since the early signs may present similarly to stress reactions.
First, respond to threats to the patient’s life by protecting their airway, supporting their breathing, and stopping any external bleeding (the ABCs). Treating an injury, such as splinting a fracture or cooling a burn, is also treatment for shock, since this may address the cause of the shock.
Next steps for shock treatment consist of maintaining the patient’s temperature within normal limits, giving fluids orally (if your patient can swallow), and elevating their legs 8-10 inches.
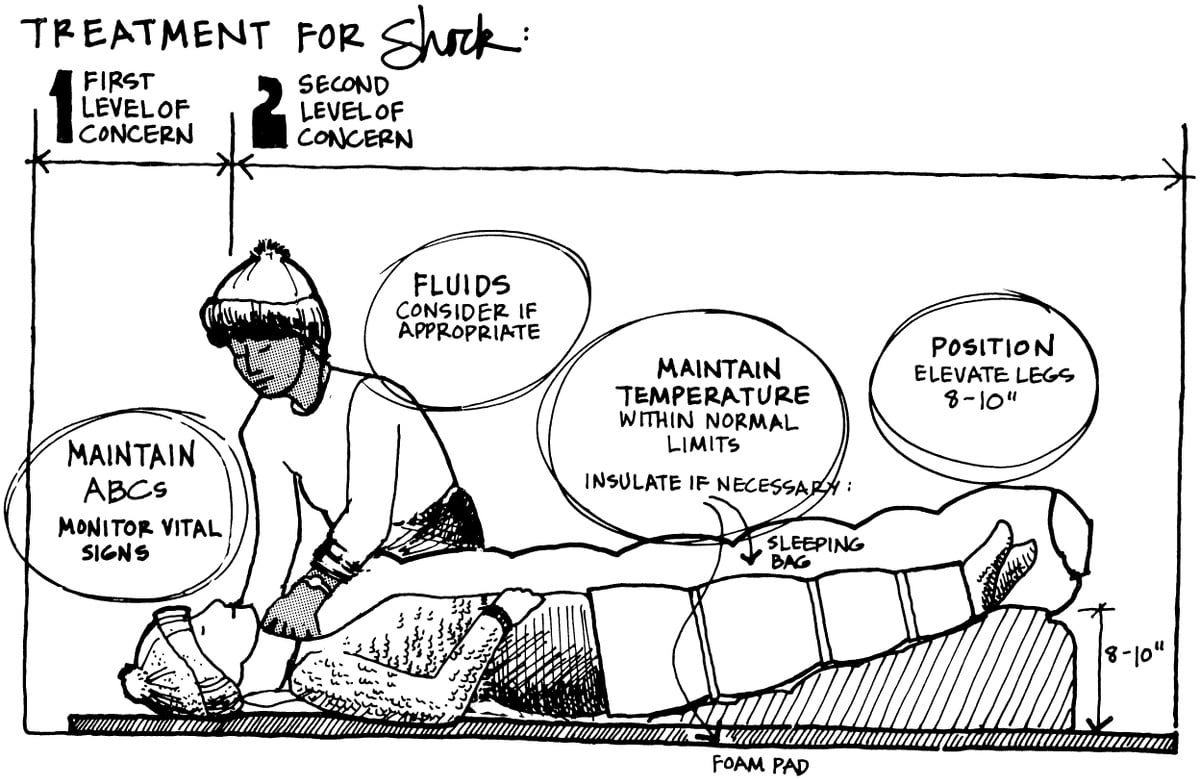
Whether the above position helps return blood to the heart is debatable, but it doesn’t harm the patient and can be used until you have assessed the problem and ruled out shock.
Evacuation Guidelines for Shock
Worsening shock, characterized by stress response-type symptoms failing to resolve, deterioration of the patient’s mental status, and the circulatory system collapsing (falling blood pressure, radial/wrist pulse becoming weak or absent) is difficult, if not impossible, to treat in the backcountry.
While all the above treatments can be useful for field management, the definitive treatment for shock is evacuation. Evacuate any patient whose vital signs do not stabilize or improve over time, and do so rapidly if the patient has decreased mental status or deteriorating vitals.
Written By
Ben Lerman
Ben is the former NOLS Wilderness Medicine Marketing Coordinator and a Wilderness First Responder graduate. He enjoys rock climbing, backpacking, kayaking, and hopes to someday adventure in the mountains on each of the 7 continents.



